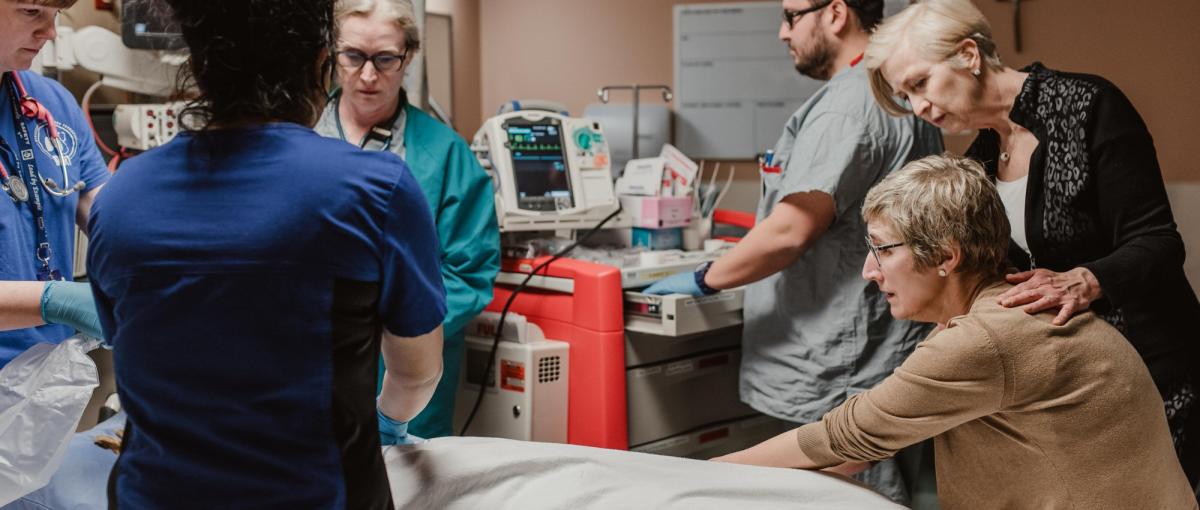
Family presence during life-saving measures
Relatives can choose to stay or leave during resuscitation efforts
February 26, 2018
By Tessia Verbeek, Senior Advisor, Communications, Covenant Health
When a hospital patient stops breathing, you may expect family members to be hurried out of the room so the medical team can begin emergency resuscitation.
That’s not the case at Covenant Health, where families are given the choice to stay bedside with their loved ones during certain crises, like respiratory or cardiac arrests.
And having that choice is important, says Glen Peterson. His wife, Sherry, who often requires medical care for her multiple sclerosis, was recently admitted to the Misericordia Community Hospital (MCU) Intensive Care unit due to respiratory issues. Glen quickly realized how urgent this visit was.
“Sherry couldn’t clear her lungs and they were filling up with fluid,” says Glen. “She was hooked up to a ton of machines. It was overwhelming. Between all the equipment and people in there, the room was filling up fast. I saw the crash cart coming and thought, ‘Well, this can’t be good.’”
Sherry had respiratory failure. Her lungs had stopped working and she couldn’t breathe.
“I thought, ‘The last thing these doctors need is me in the way,’” says Glen. “I found a chair outside and sat down. A very nice lady sat down next to me and started talking—just explaining as best she could what was going on.”
The person speaking with Glen was a family presence facilitator. This individual can be a chaplain, senior nurse or cardiologist; whatever the title, this Covenant Health employee is dedicated to the family of a patient during resuscitation efforts.
“The fact was, it was pretty serious,” Glen continues. “She gave me the option of going into Sherry’s room … but I just wanted to get out of the way.”
“Families should be given a clear explanation of what they’re walking into as well as the choice to come in or wait outside,” explains Sarah Kosowan, Nurse Practitioner at the Misericordia.
Part of that explanation includes the stipulation that relatives must respect staff if they ask them to leave at any point.
“We will explain why, like if the room needs to be sterile or the relative becomes too distraught,” says Sarah.
Ideally, conversations about treatment and life-extending care happen before an emergency.
“Advance care planning is important at every age and stage of health,” says Sarah. “When family is involved, resuscitation efforts aren’t as prolonged, because in many cases, family members will stop us and say, ‘This isn’t what my loved one would want.'''
Whether relatives want to stay or leave, the medical team works to facilitate that choice.
“When they stay, family members can heal and grieve better, because they see with their own eyes the effort that went into saving their loved one,” says Sarah.
A common misunderstanding is that families who witness resuscitation would find the experience too traumatic or would get in the way of care.
“It’s actually the opposite,” says Sarah. “It’s when there is no information shared that the experience becomes traumatic or stressful. Plus, families are a powerful reminder to the healthcare team that the person whom they are treating is a real person and part of a family. Family presence doesn’t interfere with our care; it enhances it.”
Despite not going into the room during Sherry’s respiratory arrest, Glen was actively involved, thanks to the family facilitator.
“A few minutes later, someone said Sherry was going towards recovery,” shares Glen. “I said, recovery—that’s the best word I’ve heard all day.”
Sherry is now back home with Glen.
“The staff, Sherry’s doctor—they never gave me false hope,” Glen says. “I felt like part of the team. I appreciate that.”