Aesthetic breast cancer surgery gives women options
Surgeons at the Misericordia Community Hospital are at the forefront of oncoplastic approach to breast cancer treatment.
November 18, 2021
By Marguerite Watson, Senior Communications Advisor, Covenant Health
Jane Smith is grateful she was able to have oncoplastic surgery as the treatment for her breast cancer at the Misericordia Community Hospital last March. The stage 0 cancer — a non-invasive form of the disease in which abnormal cells are confined to the milk ducts — had been missed through a screening mammogram and was found through a breast MRI.
“To have that option, and to have caught this cancer at the stage it was at, I just feel so blessed,” says Jane, 49.
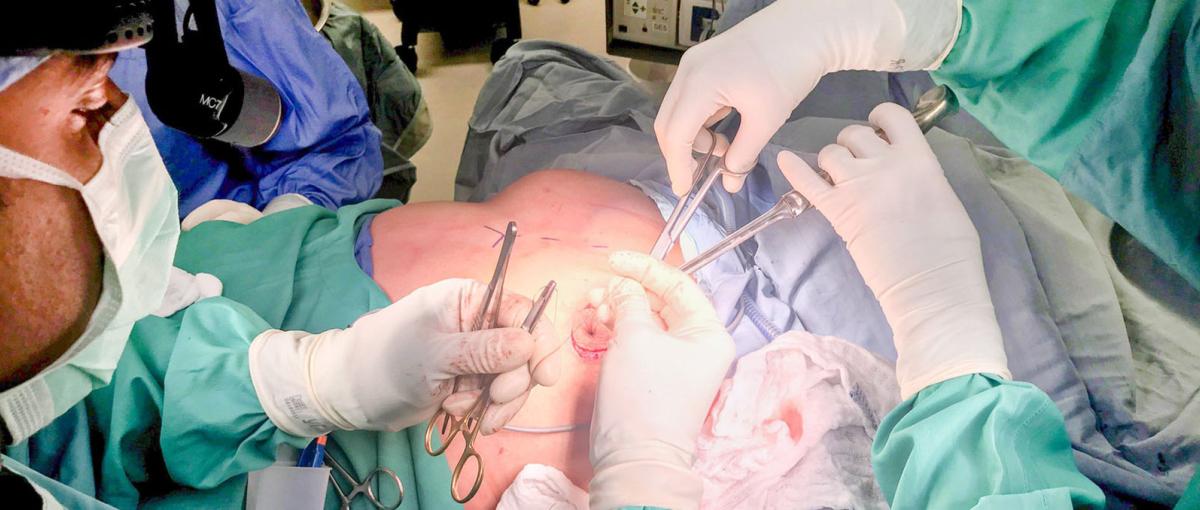
Oncoplastic breast conserving surgery is an aesthetic approach to breast cancer treatment. Through this approach, a surgeon removes the malignant tumour and reconstructs the defect, or hole, remaining in the breast to give the patient the best possible cosmetic result. While this type of surgery has been a standard of care for patients in Europe for many years, it is becoming increasingly available in North America. And a group of four full-time breast surgeons at the Misericordia — who treat about 700 patients a year — are at the forefront of oncoplastic practice in Canada.
Historically, patients had few options for surgery, but now many are able to choose oncoplastic breast conserving surgical techniques over having a mastectomy, says oncoplastic and reconstructive breast and general surgeon Dr. Lashan Peiris, who completed Jane’s surgery.
“There used to be this dogma that if a tumour is five centimetres or greater, you have to have a mastectomy. And now, we challenge that dogma. We regularly take out tumours of five, six centimetres and preserve the breast because we know that we can reconstruct the defect left behind.”
Lashan and his colleagues — Dr. Nikoo Rajaee, Dr. David Olson and Dr. David Lesniak — make up the Alberta Breast Surgical Oncology (ABSO) group, which serves the oncoplastic program at the Misericordia.
”Our ABSO group takes an oncoplastic approach in all our cases,” says Nikoo, an oncoplastic breast surgeon who was recruited to the group from Ontario in 2019. “We all try to fill the defects, and the goal of oncoplastic breast surgery is to provide the best oncologic and cosmetic outcomes for the patient.”
The surgery can take different forms depending on the size and location of the tumour, says Lashan. The simplest form, or level 1, involves removing a small cancer and closing the hole left behind, taking care to place the surgical incision where it will be least visible. A level 2 operation means removing 20 to 50 per cent of the breast tissue and using more specialized techniques, such as a reduction, to give the breast as good a shape as possible.
Jane had level 2 oncoplastic surgery. It was a two-step process: first, a procedure to assess the lymph nodes for any cancerous cells and second, a procedure to remove the cancerous breast tissue and lift, reduce and shape both breasts to maintain symmetry.
“I was a large-breasted woman, so I was ideal for that type of surgery,” says Jane. “The results are good. My clothes fit better. I feel a little bit healthier. There are a lot of advantages to reduction.”
For patients who need or choose a mastectomy or have more complex cosmetic issues, Lashan, Nikoo and their colleagues work with or refer to plastic and reconstructive surgeon Dr. Paul Schembri and his colleagues at the Misericordia, who may perform a breast reconstruction using an implant or other surgical technique.
“I think what’s really changed in the last couple of years is thinking about where the breast cancer is and determining the simplest thing we can do to rid this patient of the tumour and also remove the negative stigma of the actual surgical encounter they’ve had,” says Paul.
Research shows that the cosmetic outcome of breast cancer surgery affects patients’ quality of life. Women report increased overall happiness following good results or once they’ve undergone breast reconstruction. Those who experience poor results or haven’t had a reconstruction report more depression and worse emotional and psychological side effects.
Acknowledging the emotional and psychological impacts is extremely important, says Nikoo. “It’s our responsibility as surgeons to consider how our patients will feel when they look at themselves 10 years from now and to do whatever we can so they don’t have a constant reminder of their cancer and the trauma associated with it.”
She urges women who are over 50, and those who are under 50 and at higher risk of developing breast cancer, to have regular mammograms and in some rare cases, such as Jane’s, further screening through a breast MRI. Both help physicians identify tumours earlier, leading to more surgical options, smaller operations and shorter cancer journeys.
Jane’s MRI was prompted by a family history of breast cancer and the recent loss of her mother to a cancer in the chest area that emerged 20 years after having a mastectomy.
“I’m very thankful at the end of the day for this life-saving operation and that my life was likely extended instead of cut short,” says Jane.